In the world of wearable health devices, sleep trackers have become a popular way for us to monitor our nightly shut-eye. There are many options for sleep-tracking technology, and plenty of people take advantage of them.
But that number pales in comparison to the number of people who sleep next to another human being — the OG sleep tracker, if you will. They may not fit on your wrist, but they can offer lots of beneficial information that’s just as valuable as what you get from your sleep tracker.
What Do Sleep Trackers Do?
Many of my patients use sleep trackers. The most popular ones I see are the Oura Ring (which I use) and WHOOP, along with other wearables that include sleep-tracking capabilities, like Fitbit and Apple Watch.
Using similar technologies, these devices all keep tabs on metrics like heart rate, heart rate variability, movement, and oxygen level, and provide good data on the stage of sleep you’re in. The result is an in-depth analysis of the duration of sleep, wake times, and time spent in each sleep cycle.
Sleep trackers also measure latency, or the time it takes you to fall asleep after you lie down. I’ve previously addressed the importance of the onset of sleep to the architecture of your night’s sleep cycle.

Too Much of a Good Thing, or Not Enough?
Sleep trackers are good at what they do, which is to provide you with data. Sometimes, there’s simply too much data. On some mornings, I open my Oura app, see three or four graphs and four or five percentages, and think, “I don’t have time for this!”
The data is also very complex — making it difficult to quickly analyze. It’s not that the data is wrong; it’s that the course of action needed to address it may not be clear. And data without action is useless.
Despite all this potentially useful information, the data can be easy to dismiss due to its amount and complexity.
DOWNLOAD OUR FREE EBOOK
Concierge Medicine is the future of healthcare.
Learn more about this refreshing alternative to traditional primary care, and decide if it's right for you.
Key Considerations to decide...
Is Concierge Medicine Right for You?
Your spouse, on the other hand, is harder to ignore. They might say, “I’m worried about you. You don’t seem well rested in the mornings.” Or, “I’ve noticed you seem to gasp for air at night.” That can be more impactful than a report on your phone.
If you get a poor sleep score from your tracker, ask why. Look at the big picture and take a moment to reflect on the prior day (or days). How was your nightly routine? What changed from night to night or from weekday to weekend? What actions can you take to evaluate these influences on your sleep score?
Maybe you notice that your sleep score dives into the 70s when you drink a glass of wine two hours before bed. Now you have an action item: Don’t drink wine before bed.
It takes some thoughtful consideration to identify the factors that affect your sleep and act on them. It’s not nearly as easy as slipping on a wearable at bedtime, but it’s absolutely necessary if you want to apply the data you’re tracking.
Don’t Dismiss Your Partner’s Feedback
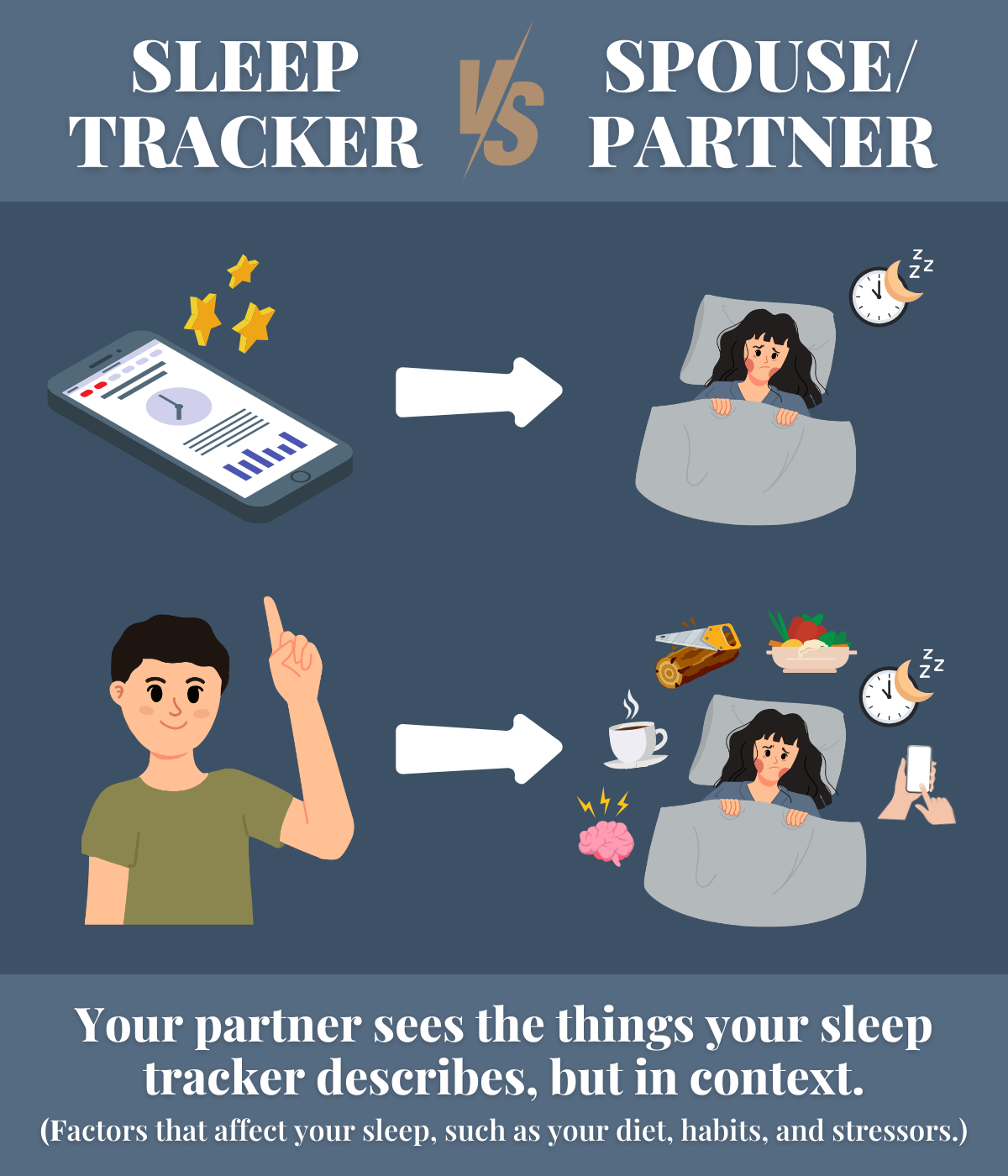
Your sleep partner is going to understand — and likely be involved in — the factors that affect your sleep, such as your diet, habits, and stressors. They’re going to see how your lifestyle choices manifest at night. Are you lying in bed too long, staring at the ceiling? Are you restless? Are you snoring or struggling to breathe? (These can be signs of an underlying sleep disorder!)
Your partner sees the things your sleep tracker describes in context. And when they offer input, they’re able to do so with love and compassion, which your sleep tracker can’t. They love you and want what’s best for you. Plus, you don’t have to pay them a monthly fee, and they don’t stop working if you fail to download the latest update.
If you’re wearing a sleep tracker, you’re likely serious about your health, and you take responsibility to optimize it. Just remember: Technology is not your only resource. Be open to feedback from the people in your life — especially your spouse — because they have insights you can’t see.
Sleep Apnea: Overlooked and Underdiagnosed
Your spouse is your partner in life and, therefore, in health. If you develop a sleep disorder, it’s unlikely you’ll be able to detect it yourself. But your spouse could very well see the signs.
The two most common sleep disorders I encounter are obstructive sleep apnea (OSA) and psychophysiological (stress- or mood-induced) insomnia. If you’re suffering from insomnia, you likely know it. But that’s often not the case with sleep apnea. Again, this is where your partner’s feedback can be invaluable, but only if you take advantage of it.
For example, snoring is practically a cultural punchline, and it’s easy to brush off a partner’s complaints with a laugh — or with indignation (“Well, you’re just a light sleeper!”).
Remember, you can’t gauge your activity while you’re asleep. If you have sleep apnea, you won’t detect it on your own. You likely won’t recognize the extent of your snoring, and you probably won’t wake to full consciousness during apneic episodes. But your partner can pick up on your snoring, irregular breathing, and other signs.
Obstructive sleep apnea is not only a vastly underdiagnosed sleep disorder; it’s also largely misunderstood. Sleep apnea isn’t just about disruptive snoring or daytime sleepiness. Sleep apnea is dangerous, and it’s a killer.
Uncontrolled sleep apnea leads to high blood pressure, insulin resistance, vascular disease, heart failure, and hormone imbalance — particularly low testosterone. It’s a serious disorder, and it needs to be treated as soon as possible to curtail its effects on your health.
Risk factors for sleep apnea include excess body weight, a large neck size, and a small airway. Alcohol and some sleep medications can exacerbate apnea.
Symptoms of sleep apnea include morning sluggishness, low energy, forgetfulness, ongoing fatigue, the need for naps, and poor mental focus. But it goes beyond this. You may find yourself feeling angry, frustrated, or even having trouble in your relationships. Remember, if you have sleep apnea, your partner’s sleep cycle is likely being interrupted as well, which can cause stress and friction.
Signs, Symptoms, and Treatment
Loud snoring or otherwise disordered sleep can lead couples to sleep in separate rooms. They may start out in a shared bed, but one eventually migrates to the couch or the spare bedroom. While this may seem innocuous, I’d like to emphasize that it indicates a real problem.
Patients may not immediately mention something like this to their doctors, but it’s a significant piece of information that lets us know a person needs to be screened for obstructive sleep apnea.
I can’t overstate the significance and impact of sleep apnea. Though some risk factors, such as weight, are correctable with lifestyle changes, the effects of OSA are serious enough that treatment is needed while you take such steps.
In other words, fix the problem while you address the origin. Don’t wait to get your weight under control before doing a sleep study. Early detection and intervention can really advance your health, even in the short term.
Treatment for sleep apnea usually involves the use of a CPAP machine, oral appliance, or various other devices.
Final Thoughts
As in all concierge medicine, we would much rather look ahead in prevention than look back with regret. If you use a sleep tracker, great! But remember that a spouse is the OG sleep tracker. Listen to their feedback and be upfront with your doctor. It could save you a world of regret in the future.
At the end of the day — literally! — healthy sleep equals a healthy you.

Dr. Wright joined Brentwood MD in 2022 as the model allows him to spend more time connecting with patients and build a foundation of exceptional care. He is a Nashville native and completed his family medicine residency at the University of Tennessee Health Science Center, where he also served as Chief Resident. He believes that your health deserves a prominent position on your priority list, and would be honored to serve you and your family.